This tutorial will take you through the sequence of events in the life cycle of a red blood cell.
You can navigate through this tutorial using the buttons at the top of the screen.
The tutorial will ask you questions. Click on your chosen answer to see feedback; click the answer again to make the feedback disappear. When you're finished with one page, click the navigation button for the next page to move ahead.
Have fun! Click on button '1' to see the first page of the tutorial.
Page 1
Erythropoiesis
Red blood cells are the workhorses that carry oxygen to your body. You have to keep an adequate level of these cells in your blood, or the tissues suffer from lack of oxygen.
Red blood cells, like other blood cells, are made in the bone marrow. This process is called erythropoiesis.
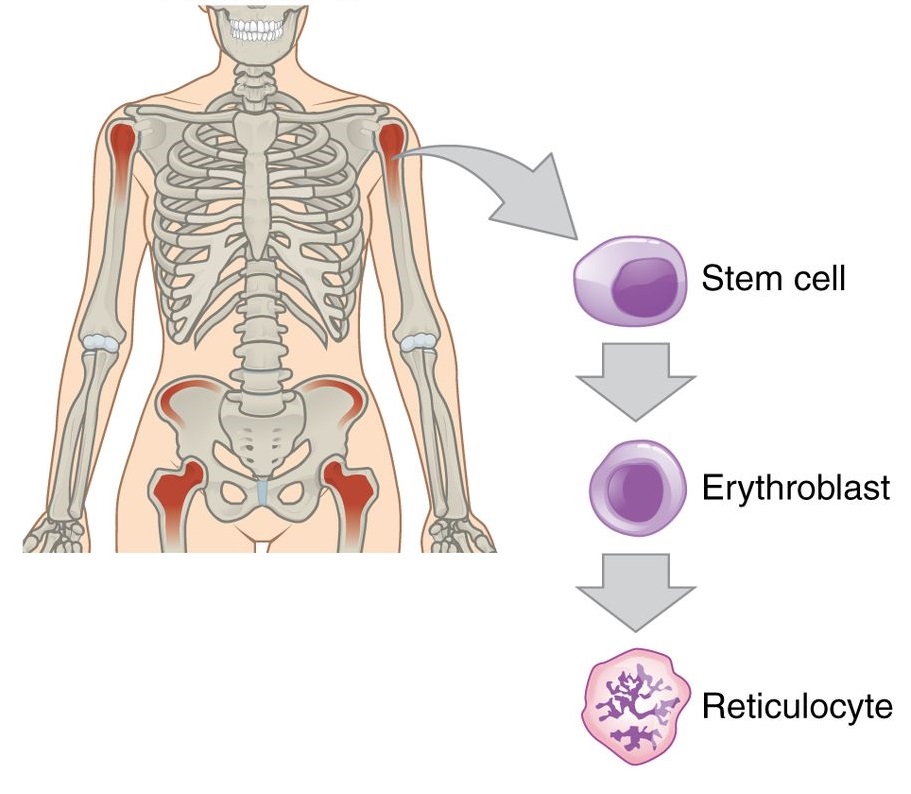
modified from an image by OpenStax College, via Wikimedia Commons. Used under a Creative Commons license.
Red blood cells are formed by stem cells in the bone marrow, but they are very different from stem cells. Since their only job is to carry oxygen around, red blood cells don't need very many organelles. As they develop, they begin to lose their organelles until all they have left is the endoplasmic reticulum (ER) - the place where proteins are made. The ER is busy making hemoglobin, the oxygen-carrying protein which fills up the space where all the other organelles used to be.
At this point the cell is called a reticulocyte, and it can be released from the bone marrow into the blood stream. In a healthy person, 0.5-1.5% of the red blood cells out in the circulation are reticulocytes 1. An elevated level of reticulocytes indicates that the bone marrow is making RBCs more quickly than usual, pushing them out before they are mature.
Mature red blood cells, or erythrocytes, have lost the endoplasmic reticulum and are essentially just bags of hemoglobin.
1Gerston, T. (2014) Reticulocyte Count. Retrieved from Medline plus at https://www.nlm.nih.gov/medlineplus/ency/article/003637.htm.
Page 2
A common way to measure RBCs is by centrifuging a blood sample so the cells fall to the bottom of the tube. Then you can just measure the height of the RBCs and the height of the total sample and figure out what percentage of the blood is made up of RBCs -- the hematocrit.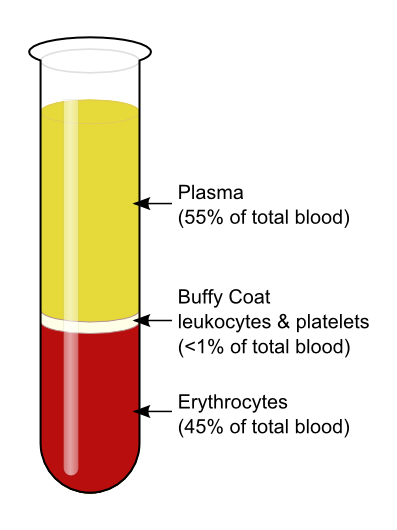
Knudsen, K (2008) at English Wikipedia, via Wikimedia Commons. Used under a Creative Commons license.
Normal hematocrit levels are around 42%-54% in adult males and 38%-46% in adult females.1 But what maintains the hematocrit? How does your bone marrow know whether it needs to make more RBCs?
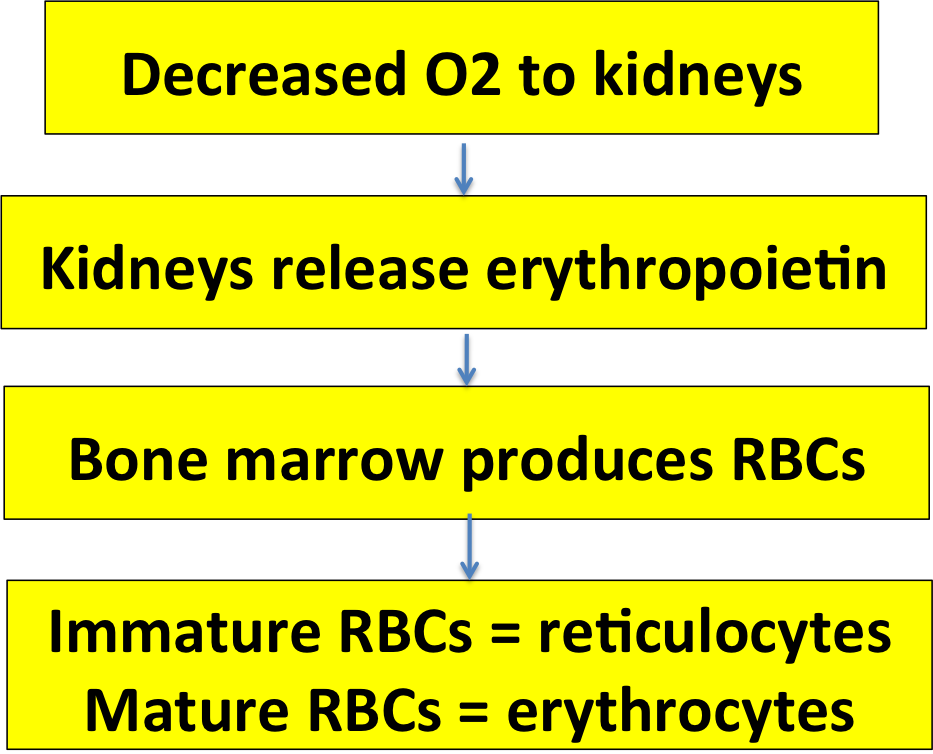
If the number of RBCs decreases, the amount of oxygen carried to the tissues will decrease. That's what clues your body in to the need for more RBCs.
The kidneys are the tissues that cause the bone marrow to make more RBCs. When the kidneys lack oxygen they release the hormone erythropoietin, which stimulates RBC formation in the bone marrow.
1Davis, C. P. (2014). Hematocrit. Retrieved June 3, 2016, from emedicinehealth.com.
Page 3
Time for a review. Choose the right words to fill in the blanks!
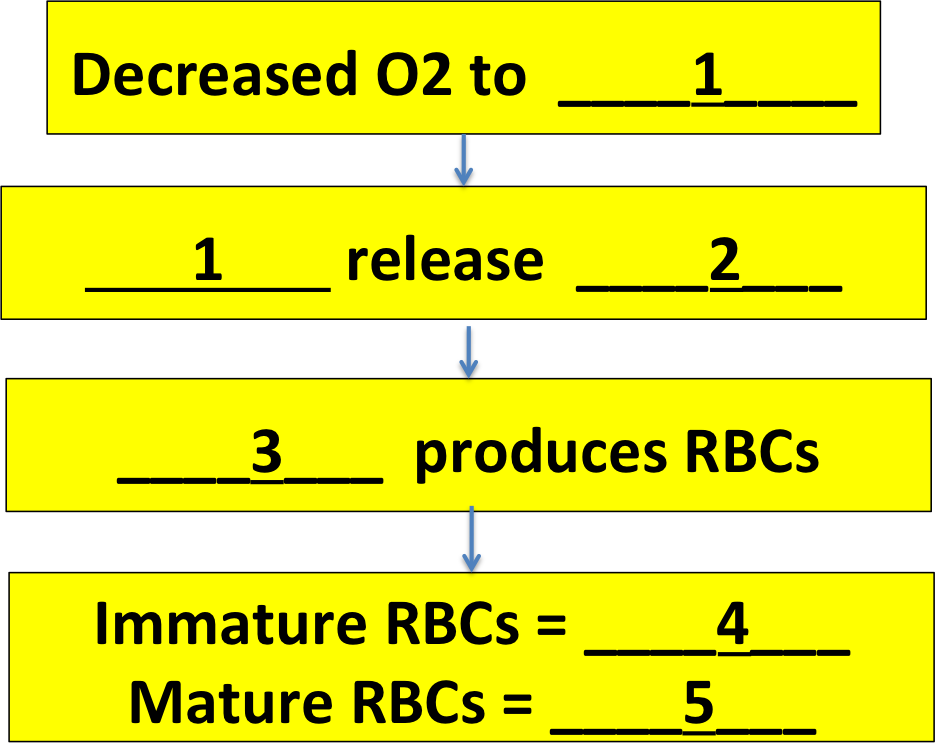
1 should be: kidneys / tissues / bone marrow
2 should be: oxygen / erythropoietin / erythrocytes
3 should be: kidneys / spleen / bone marrow
4 should be: erythrocytes / stem cells / reticulocytes
5 should be: reticulocytes / erythrocytes / stem cells
Page 4
Page 5
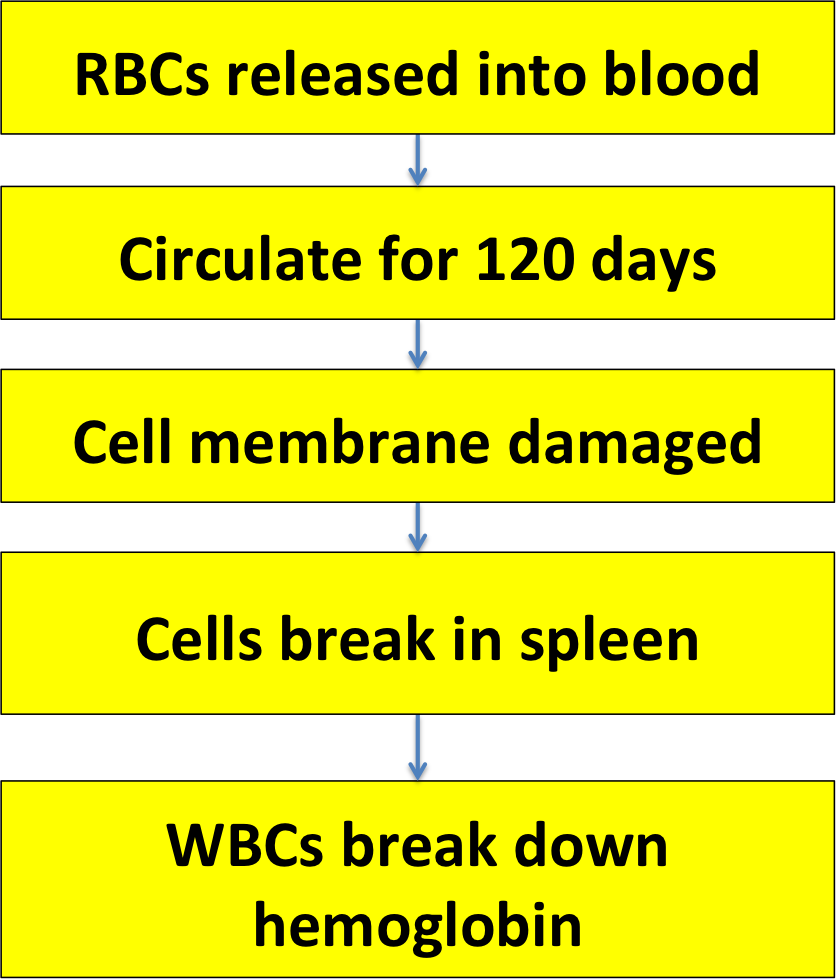
RBCs don't live very long, because they have a hard time out in the circulation. The biggest challenge they face is going through capillary beds. Look at how these RBCs are being deformed and squashed!
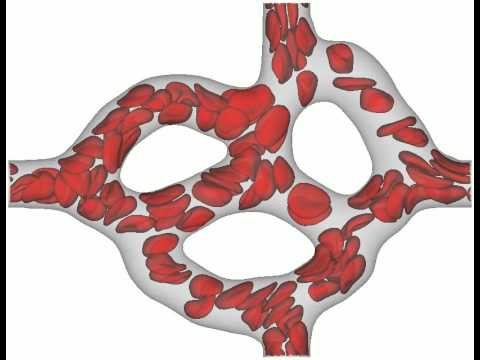
Gambaruto, A. (2015). Simulation of red blood cell movement through a retinal capillary. Youtube. Used under a Creative Commons License.
Lots of things start to go wrong with RBCs as they age, and some make the cells more likely to break down or die. For example, older RBCs tend to be more rigid, less able to bend or fold as they squeeze through the capillaries. Other changes 'mark' the aging cells and make white blood cells more likely to attack them.1
1Antonelou, M. H., Kriebardis, A. G., & Papassideri, I. S. (2010). Aging and death signalling in mature red cells: from basic science to transfusion practice. Blood Transfusion, 8(Suppl 3), s39–s47.
Page 6
Destruction of Old RBCs
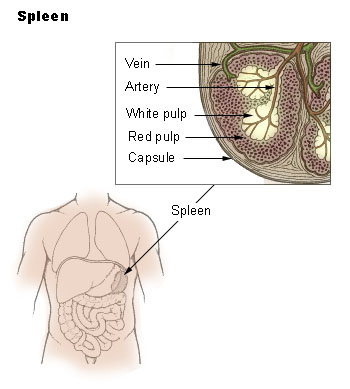
National Cancer Institute SEER training modules (n.d.) Spleen. Public domain image.
Your spleen is like a giant lymph node, full of white blood cells; but it also contains some tissue called red pulp, in which it stores and processes RBCs.
How did it get those RBCs? They came from the circulation. The spleen is filled with special capillaries called sinusoids. They have large gaps in their walls, big enough for RBCs to leak out and into the spleen's red pulp.
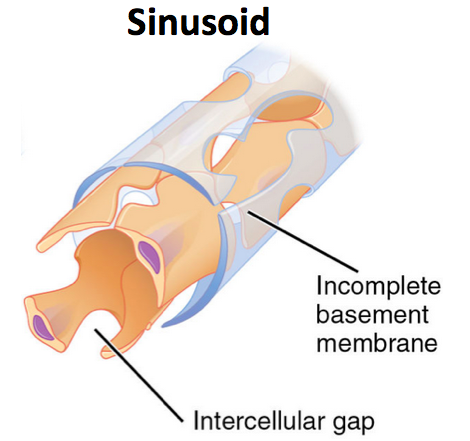
Modified from Anatomy & Physiology, Connexions (2013) Depiction of the major types of capillaries. Wikipedia. Used under a Creative Commons License.
When the RBCs have leaked out into the spleen, they can stay there for a while. That's how the spleen stores RBCs, in case you suddenly need them. Also, the RBCs can interact with macrophages, WBCs living in the spleen. The macrophages can actually help repair damage to the RBCs!1 But if the RBCs are too damaged, and too stiff and old to get back into the sinusoids, the macrophages will destroy them.
1 - Back, D. Z. de, Kostova, E. B., Kraaij, M. van, Berg, T. K. van den, & Bruggen, R. van. (2014). Of macrophages and red blood cells; a complex love story. Frontiers in Physiology, 5.
Page 7
Bile Pigments
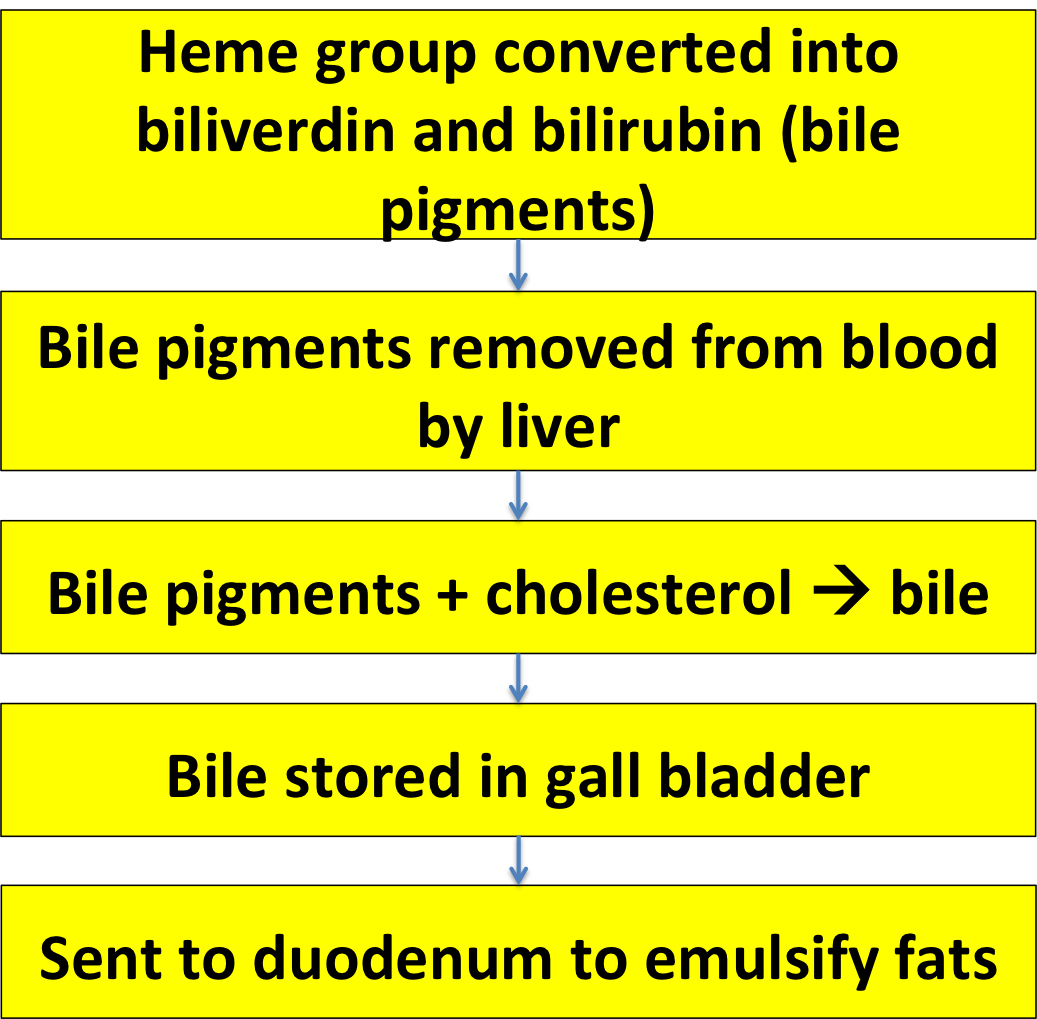
When RBCs break open, hemoglobin gets out. Hemoglobin can be toxic, so the macrophages convert it into two less dangerous compounds: biliverdin ('verd' means green) and bilirubin ('rubin' means red, though bilirubin is actually more of an orange-brown color).
Modified from Kübelbeck A. (2011).Wikipedia. Used under a Creative Commons License.
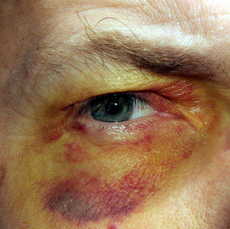
You can get a look at these compounds the next time you have a bad bruise. It will be red in the beginning because of hemoglobin from broken blood vessels, and then black/blue as the hemoglobin becomes denatured; then you'll see the bruise become yellow-greenish as hemoglobin is converted into biliverdin and bilirubin.
People with too much bilirubin in their blood can develop this coloration all over their bodies (jaundice) or in the whites of their eyes (icterus).
The bile pigments are removed from the body by your liver, which combines them with cholesterol to produce bile. The bile is then stored in the gall bladder until you eat some fat: then your duodenum releases the hormone cholecystokinin, which makes the gall bladder contract and shoot the bile into the duodenum, where it is used to help digest the fats.
Page 8
You know what to do…
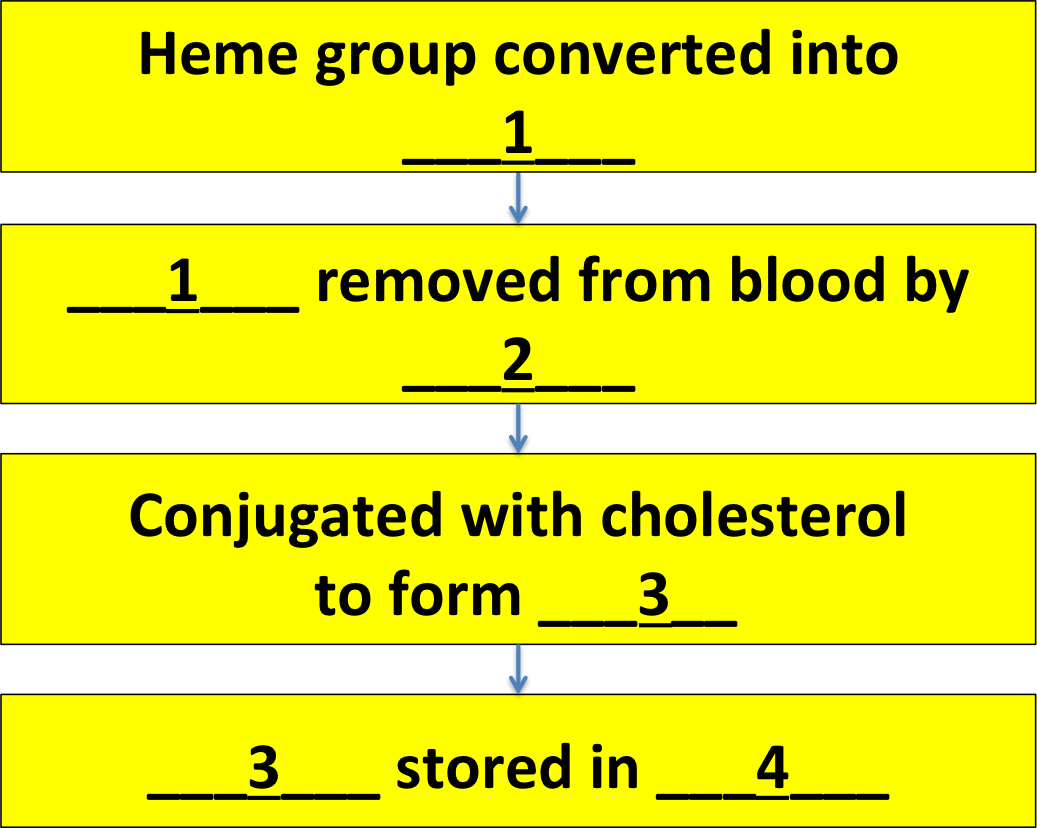
1 should be: bile / bilirubin and biliverdin / erythrocytes
2 should be: kidneys / spleen / liver
3 should be: bile / bilirubin / heme groups
4 should be: bone marrow / liver / gall bladder
Page 9
Good work. Here's a summary of the RBC life cycle for your notes.